ZapEHR and HEDIS Data Collection: A Custom Solution for Startup Practices
Health tech startups using ZapEHR can automatically generate HEDIS reports, relieving them from the compliance burden of submitting annual HEDIS metrics required by insurance billers.
TL;DR - All organizations that bill insurance must submit HEDIS metrics because HEDIS reporting is an annual obligation for payers. Applications built on ZapEHR can generate HEDIS reports automatically (subject to NCQA approval) greatly reducing the compliance burden on health tech startups.
More than 200,000,000 people are members of insurance plans required to report quality data via the Healthcare Effectiveness Data and Information Set (HEDIS). HEDIS are a core group of measures which evaluate care quality and efficiency across six domains. As of 2023, there are more than ninety measures under HEDIS. These criteria, set by the National Committee for Quality Assurance (NCQA), track the provisioning and impact of care, as well as disease prevention and management across members’ lives. NCQA includes representatives from plan purchasers, providers, and consumers.
HEDIS monitors the health of plan populations and evaluates performance of participant providers and health plans. Many plan incentive programs available to providers are HEDIS metric-based pay-for-performance.
Startups providing health services and billing insurance plans are not exempt from HEDIS data provision requirements. Every organization that bills insurance for services, no matter how new or small, is subject to periodic HEDIS assessment.
HEDIS reporting is a requirement for health plans themselves to maintain accreditation and regulatory compliance both through NCQA and the Centers for Medicare and Medicaid Services (CMS). Both commercial and Medicare/Medicaid plans are impacted by HEDIS reporting. Because HEDIS covers so many lives, it is one of the largest surveys in managed care.
HEDIS is evaluated across six domains of care:
Effectiveness of Care
Access/Availability of Care
Experience of Care
Utilization and Risk Adjusted Utilization
Health Plan Descriptive Information
Measures Reported Using Electronic Clinical Data Systems
Within each group are measures in areas such as prevention, screening, systems-based assessments, visit completion, and utilization.
Data Collection
Given the wide scope of HEDIS measurement, data is collected in three ways.
Surveys - Such as the Consumer Assessment of Healthcare Providers and Systems (HCAHPS) which enables plans to monitor patient satisfaction
Administrative Data - Information generated as a byproduct of care such as claims, office visits, or pharmaceutical utilization
Hybrid Data - Where data from claims is combined with the actual medical record of the patient for greater depth into performance measure completion.
ZapEHR can programmatically ingest and store this data for synthesis into measured performance calculations*. For portability across systems, ZapEHR is capable of mapping data elements into FHIR-compliant resources as well as accepting data from multiple sources. ZapEHR’s API directly feeds visit and claim data into a FHIR data store without the cumbersome movement of files through SFTPs or portals. This API also connects ZapEHR to health information exchanges (HIEs) for access to pertinent data across the care spectrum.
Metric Calculation
Recently, HEDIS reporting metrics have become more standardized across payers. However, there are still significant inclusion or exclusion criteria for each metric - factoring in detail such as age, previous conditions, or time intervals between included measurement types.
For example, the 2023 NCQA definition of colorectal cancer screening is described as follows:
“Assesses adults 50–75 who had appropriate screening for colorectal cancer with any of the following tests: annual fecal occult blood test, flexible sigmoidoscopy every 5 years, colonoscopy every 10 years, computed tomography colonography every 5 years, stool DNA test every 3 years.”
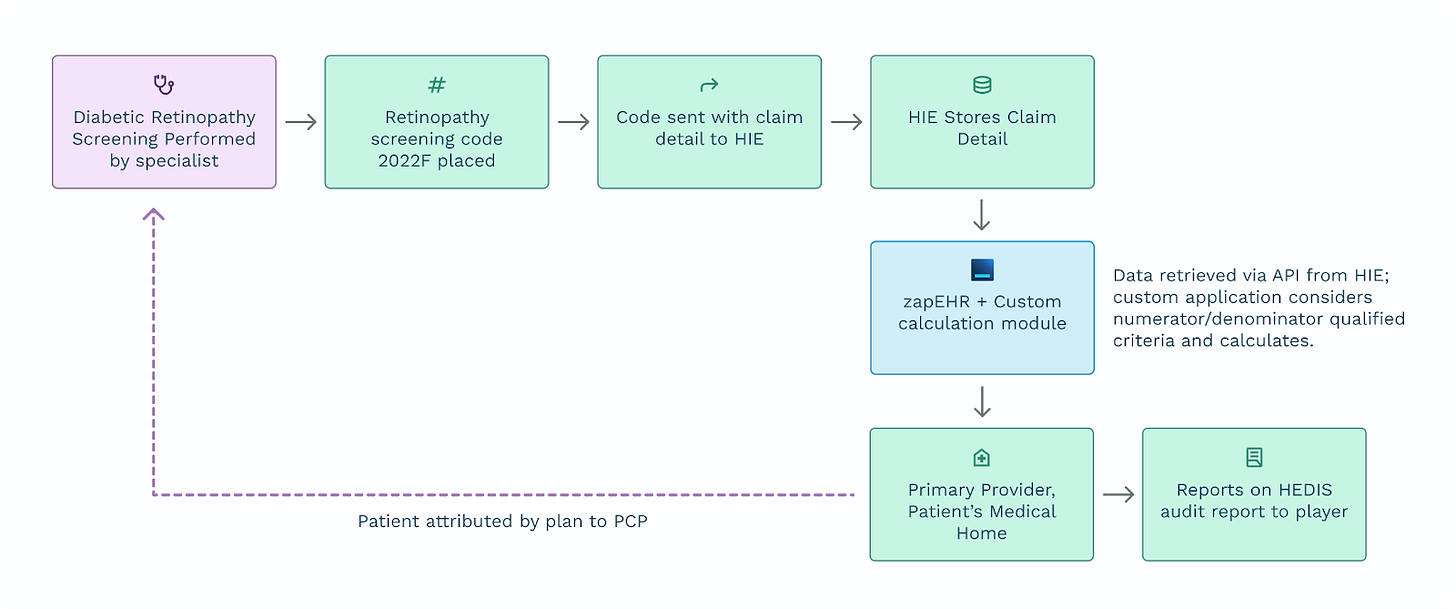
Correctly reporting this metric for a patient requires (1) an understanding of their age at the time of performance; (2) a distance between measurements and (3) a sliding scale of measurement periods compared to the next most recent procedure code found for one of three accepted methods for CR cancer screening. Without additional detail from a referring gastroenterologist or previous PCP, it may be next to impossible to accurately determine whether the patient’s metric was accomplished by CT colonography or by DNA test. Additional patient information from an HIE combined with pre-programmed calculations using ZapEHR means not only accurate payer performance reporting but also more precise patient management. The complete listing of MY 2023 NCQA measures can be found here.
ZapEHR, by its headless nature, is customizable. They are able to leverage internal datastores like any other electronic health record but also manage multiple API connections and achieve a level of flexibility using programmable functions that would be unrealistic with a monolithic EHR. This is especially useful for HEDIS or other performance metric reporting; they allow ZapEHR to ingest, retain, and calculate performance metrics both automatically and on-demand for various insurance payers. With a ZapEHR, there’s no need for clinical staff to spend time abstracting and determining inclusion/exclusion per patient during annual reporting periods.
In addition to the required measures, there are frequent updates to the HEDIS logic that require tailoring and specific adjustment to inclusion or exclusion criteria. In 2023, new cross-cutting exclusions granted exemption for members in palliative care, long-term nursing, those with advanced illness, and other exempt criteria. An HIE attached to ZapEHR may be able to detect these patient status changes and exempt the patient from the quality reporting denominator in a practice’s panel. As logic is enhanced or modified in subsequent years the programmed calculation built onto ZapEHR allows for exemption on an ongoing basis so long as the code is maintained to the current specifications.
Important Facets of Calculation and Reporting
Reporting methods for HEDIS are payer-dependent. Most payers will submit their HEDIS data directly to NCQA. Providers and practices - regardless of size - must submit their quality performance and survey results to each payer they bill. This data is generally sent via secure transfer protocol to a repository. Critically, there is a mandatory requirement for reporting any errors discovered post-submission if they exceed a 5% fixed threshold. This means the responsibility for accuracy and remedy falls upon the provider, rather than the insurance plan. Erroneous submissions are then publically reported on the NCQA website; examples can be seen here.
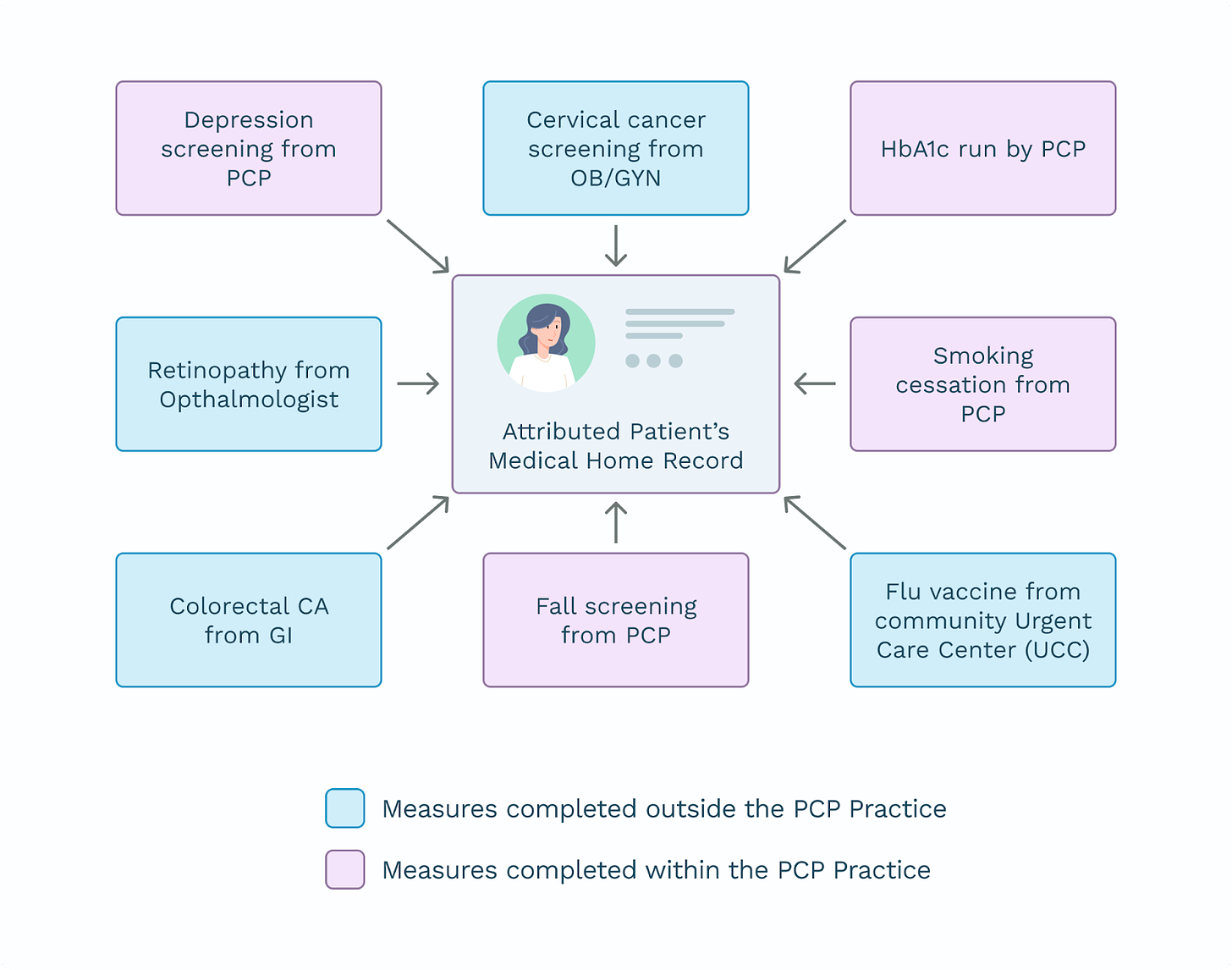
There is an important distinction between a provider or practice group finding compliance details for their own patient population versus a health plan calculating performance percentages for their member panel. For the independent or group-based provider, the objective is to use claim or visit information to determine if a measure has - or has not - been fulfilled to the satisfaction of the measure criteria. The provider is not required to calculate a performance percentage or risk-adjust the measurement themselves.
A custom ZapEHR application use bespoke code to determine if a measure has been filled per patient. In many cases the code which is used to determine HEDIS compliance must be first certified as accurate by NCQA. NCQA will provide a test deck of measures and detail, and the entity must perform measurement assessments. Once the detail is reviewed, NCQA will issue a certification for the given measure. NCQA also offers a process called Automated Source Code Review (ASCR) so provider organizations can verify their own source code with NCQA.
More information about NCQA certification can be found on this helpful web page.
A Solution in ZapEHR’s Headless Technology
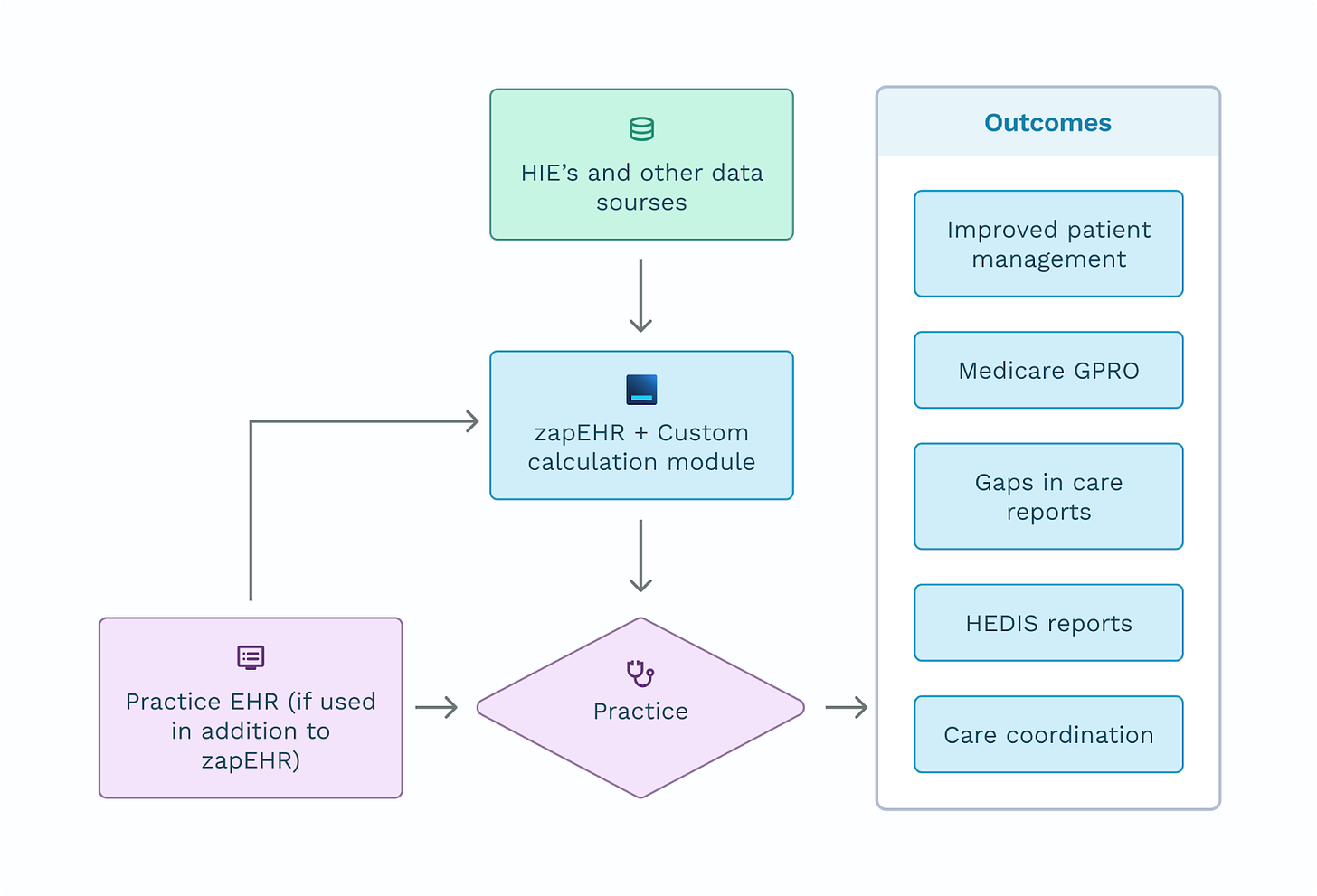
ZapEHR’s ability to populate its datastore via API to HIEs and other data sources helps providers report quality performance measures to insurance payers under HEDIS. The ability to ingest, organize, and store detail across the care team may also facilitate improvements in total patient management. Additionally, ZapEHR offers flexible solutions to program applications on top of stored data including calculating HEDIS compliance measures for submission to the health plan. Though these measure calculations may require certification through NCQA, the process to do so is straightforward and achievable for an efficient and automated result to ongoing reporting requirements.
Contact the team at ZapEHR today at info@zapehr.com and learn more at zapehr.com.
*Note that all metric calculations are user-defined, user-programmed. These may or may not be subject to NCQA certification. Consult with ZapEHR, NCQA, or the health plan to which you’ll report to learn more.